At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Exercise Urticaria?
Exercise urticaria, also known as exercise allergy, is a condition in which patients develop urticaria, or hives, in response to physical activity. This symptom is associated with two different diseases, cholinergic urticaria and exercise-induced anaphylaxis. Patients with cholinergic urticaria break into hives whenever their core body temperature rises. This is typically a mild condition that resolves on its own. In contrast, exercise-induced anaphylaxis can be life-threatening and is not triggered by alterations in body temperature.
Most often, exercise urticaria is associated with a disease called cholinergic urticaria. Patients with this condition develop a reaction whenever their body temperature rises above normal, which can occur due to exercise, elevated external environmental temperatures, or fever. The disease is most common in people in their 20s or 30s.

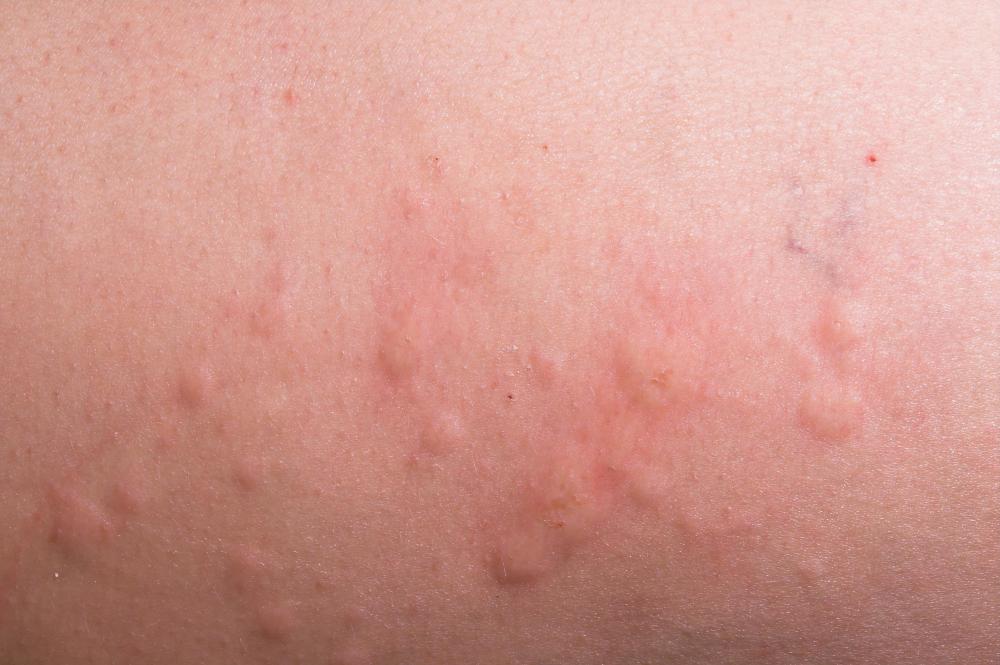
The main symptom of cholinergic urticaria is a skin rash called urticaria, a condition commonly known as hives. With this rash, many small skin lesions appear, which are composed of raised areas of skin encircled by redness. Often the rash comes on suddenly and is associated with itchiness, tingling, and pain. Occasionally patients can experience other symptoms such as dizziness, shortness of breath, nausea, and vomiting.

Typically, the diagnosis of exercise urticaria in association with cholinergic urticaria is made on the basis of clinical history. Although some tests are available to help make the diagnosis, typically doctors rely on the patient's account of symptoms and inciting events. The mainstay of treatment for this condition is to take medications in the antihistamine class. Patients should also avoid enduring conditions that are known to incite the urticaria, such as strenuous exercise. In most cases, this condition resolves within ten years of diagnosis, and patients no longer have to take medications or avoid certain situations.
Rarely, exercise urticaria can signal that a more severe condition called exercise anaphylaxis will develop. Patients with exercise anaphylaxis have much more severe symptoms than patients with cholinergic urticaria. Both conditions cause the skin rash with its associated itchiness. Exercise anaphylaxis, however, causes additional symptoms including flushing, facial swelling, lightheadedness, and fatigue. Advanced cases can cause a severe sudden drop in blood pressure that can lead to fainting and collapse.
Treatment of exercise urticaria associated with exercise anaphylaxis is mainly supportive. Patients can be given an injection of epinephrine as an immediate alleviating action. They can be supplied with intravenous fluids. Additionally, if the swelling in the neck region has sufficiently restricted the ability of the patient to breathe, respiratory support with supplemental oxygen or mechanical ventilation might be needed until the patient recovers.
Distinguishing between exercise urticaria associated with cholinergic urticaria versus that associated with exercise anaphylaxis can be difficult. Often the distinction is obvious in retrospect, especially if the patient develops a life-threatening anaphylactic episode. One way to distinguish them lies in understanding the triggers causing the urticaria. Cholinergic urticaria is stimulated by any rise in body temperature, whereas exercise anaphylaxis only occurs as a result of exercise and is not related to body temperature.
AS FEATURED ON:
AS FEATURED ON:











Discussion Comments
I found it interesting when the article said that most people get over the symptoms of this condition within 10 years of diagnosis and don't have to continue urticaria treatment. It's confusing why the symptoms would just disappear. However, I have heard about kids growing out of allergies, and this condition is referred to as an exercise allergy, so maybe there is a connection there. That would be an explanation for why the symptoms go away anyway.
I have a friend who has exercise induced urticaria. We take spin classes together. She is great on the bike. I can't keep up with her. I don't think anyone in class can. However, after class her cheeks, arms and legs have red spots on them. The spots don't look like what I think of when I hear the word hives, but when you look closely you can see little bumps.
After she showers and dresses the hives are all but gone. There is a little redness. She simply looks flushed from her workout. I guess her case is a mild one.
Post your comments