At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Allergic Purpura?
Allergic purpura, anaphylactoid purpura, or AP is a disease in which the capillaries, which are small, arterial blood vessels, become inflamed. This makes it a type of vasculitis, a term used to cover any type of blood vessel inflammation. Allergic purpura characteristically affects the capillaries in the intestinal tract, the skin, and the kidneys. Allergic purpura is more common among males than females and most likely to strike children between. Nevertheless, children have a better prognosis for recovery than adults.
Though the cause of AP is unknown, it often develops several weeks after a streptococcal infection, and seems to be connected to the body’s autoimmune response. It has also been linked to allergic reactions to a variety of things, including certain foods, drugs, and vaccines. It may also be caused by an allergic reaction to insect bites.

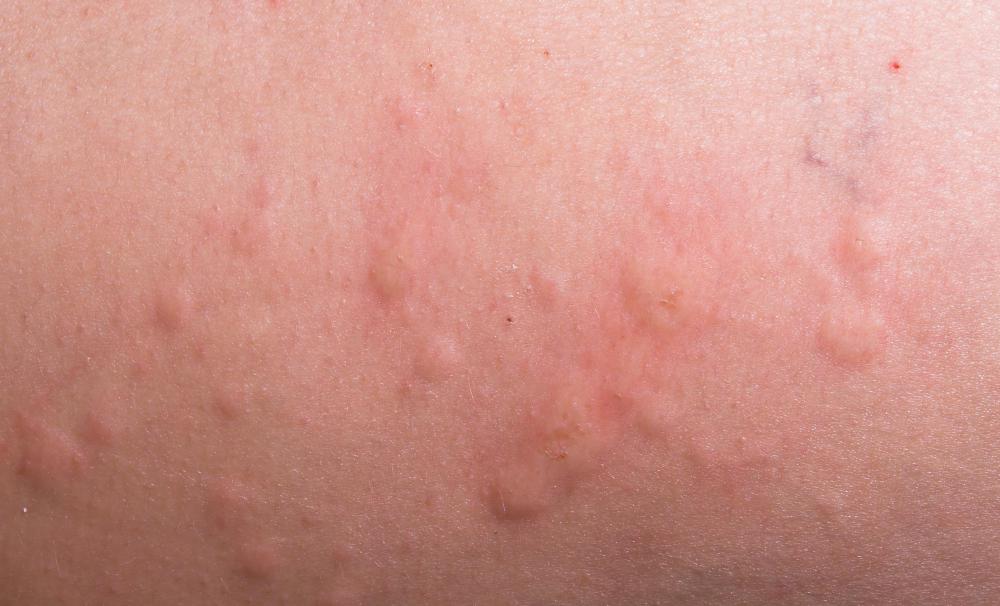
Allergic purpura may have a sudden onset or it may develop slowly, taking several weeks to fully progress. Rupturing capillaries cause the characteristic lesions—the most obvious symptom—which may first appear as areas of redness or small hives. Rash spots gradually turn purple—hence the name, which comes from the Latin word for purple—and then fade over the course of five or so days, but the rash can reoccur.

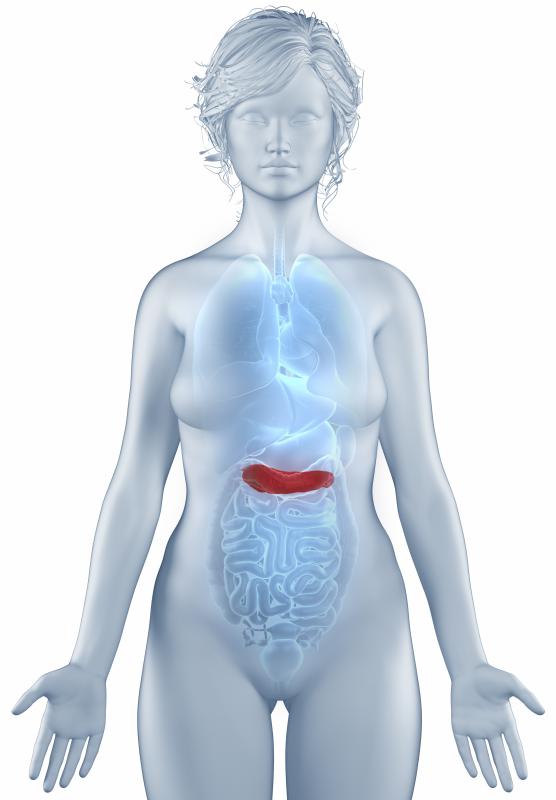
Other symptoms, indicative of more serious elements of the disease, include swelling of and pain in the joints as well as abdominal pain, due to the inflammation of the capillaries. Blood may be visible in stools and urine. Untreated, someone with allergic purpura could experience kidney failure, a heart attack, or inflammation of other organs, such as the pancreas or other problems in the renal and gastrointestinal systems. Anyone who suspects allergic purpura should see a doctor because of the severity of some of the possible symptoms.

Allergic purpura can take as long as four to six weeks to resolve, and can reoccur. Therefore, once the disease has been diagnosed and the patient is being treated, a key point will be to try to establish the cause. If it is suspected that streptococcal infection was the initiating factor, a course of prophylactic antibiotics may be prescribed to prevent a recurrence. If the cause is unclear, an elimination diet or other techniques may be used to try to pinpoint, and then permanently eliminate, a food that might have been the cause.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments